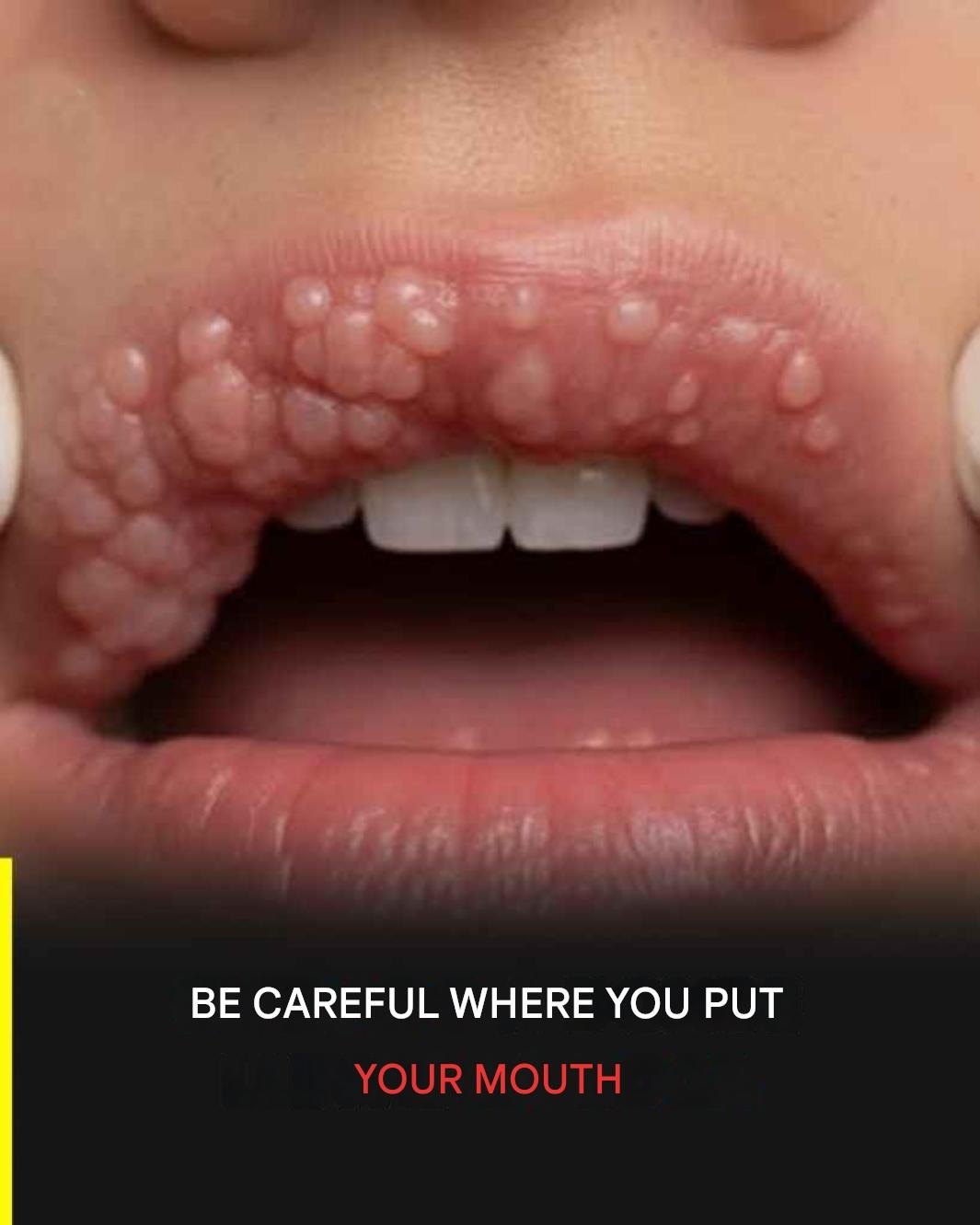
This isn’t meant to scare people. It’s meant to inform, prevent, and talk about what almost no one wants to talk about…
Human papillomavirus (HPV) is the most common sexually transmitted infection in the world. According to figures from the Ministry of Health, four out of five people will contract it at some point in their lives. Despite its high prevalence, many myths and misinformation still exist about its transmission, consequences, and prevention.
What is HPV and how is it classified?
HPV is a group of more than 100 types of viruses that affect the skin and mucous membranes. It is classified into two main categories according to its oncogenic risk:
Low-risk HPV: This type is associated with benign lesions, such as genital warts and mild cellular changes that do not usually develop into cancer.
High-risk HPV: This type includes approximately 15 types of the virus that can cause cancer, primarily cervical cancer, but also other cancers such as anal, penile, vulvar, vaginal, and oropharyngeal cancer.
Myths and Truths about HPV
Despite advances in sex education and prevention, many myths persist surrounding HPV. Debunking these beliefs is key to promoting prevention and reducing stigma.
Myth: HPV only affects women.
Fact: HPV can affect both men and women, although in men the infection often goes unnoticed because it doesn’t present visible symptoms.
Myth: You can get HPV by sharing objects, using public restrooms, swimming pools, or hot tubs.
Fact: HPV is transmitted exclusively through skin-to-skin and mucous membrane contact during sexual intercourse, whether vaginal, anal, or oral. It is not transmitted by sharing objects or through poor hygiene.
Myth: If there are no symptoms, there is no infection.
Fact: Most people with HPV don’t have visible symptoms, which facilitates its transmission without the infected person knowing.
HPV and its relationship to cancer:
HPV is the leading cause of cervical cancer. It is estimated that 99% of cervical cancer cases are related to this virus. In Latin America, the most prevalent genotypes in cervical lesions are HPV 16, present in 53.2% of cases, and HPV 18, with a prevalence of 13.2%.
Cervical cancer is the third most common cancer in women and the fourth leading cause of cancer death in young women. According to statistics from the Ministry of Health, approximately 4,600 cases of cervical cancer are diagnosed each year in Argentina, and more than 2,200 people die from this disease.
However, the impact of HPV is not limited to cervical cancer. It can also cause other types of cancer in both sexes, such as anal, penile, vulvar, vaginal, and oropharyngeal cancers. Hence the importance of knowing the methods of prevention and early diagnosis.
How to prevent HPV?
While there is no specific treatment to eliminate HPV, its consequences can be prevented. Prevention is divided into two types:
Primary prevention: This focuses on preventing infection before it occurs, using two fundamental tools:
Comprehensive Sexuality Education (CSE): Providing information on sexual and reproductive health is key to reducing the transmission of HPV and other sexually transmitted infections.
Vaccination: The HPV vaccine is included in the national immunization schedule and is administered free of charge to 11-year-old girls and boys. It is also available to other at-risk populations. Vaccination protects against the most dangerous types of HPV, significantly reducing the risk of developing cancers related to this virus.
Secondary prevention: This involves the early detection of lesions that could develop into cancer. There are two main tests for this:
Pap smear (Pap test): This detects cellular changes in the cervix before they become cancerous. It is recommended to have it regularly starting at age 25.
HPV test: This detects the presence of high-risk HPV types in the cervix. It is a complementary method to the Pap smear and is recommended starting at age 30.
If the HPV test is positive, it means the person has the virus, but not necessarily that they have developed cancer. In these cases, the Pap test helps determine if there are lesions that require treatment.
The Importance of a Comprehensive Approach:
Preventing cervical cancer and other HPV-related diseases requires a comprehensive approach that combines education, vaccination, medical checkups, and timely access to appropriate treatments. We have effective tools to drastically reduce the impact of HPV, but it is essential that information reaches everyone and that the importance of self-care is promoted.
Commitment to our health and the health of our community is key to curbing the spread of HPV and preventing serious illnesses. Individual and collective responsibility plays a fundamental role in eradicating this virus and its consequences. Information is our best tool for acting in time and making informed decisions about our health.